The impact of opioids on the central nervous system.
The Central Nervous System and Opioids
The central nervous system (CNS) is pivotal in orchestrating the myriad activities of the human body. Comprising the brain and spinal cord, the CNS stands as the principal processing hub for neural interactions. When opioids are introduced into this intricate biological framework, they elicit both beneficial and potentially harmful effects. The following expansion seeks to elucidate the various facets by which opioids interact with the CNS and their subsequent impacts.
How Opioids Interact with the CNS
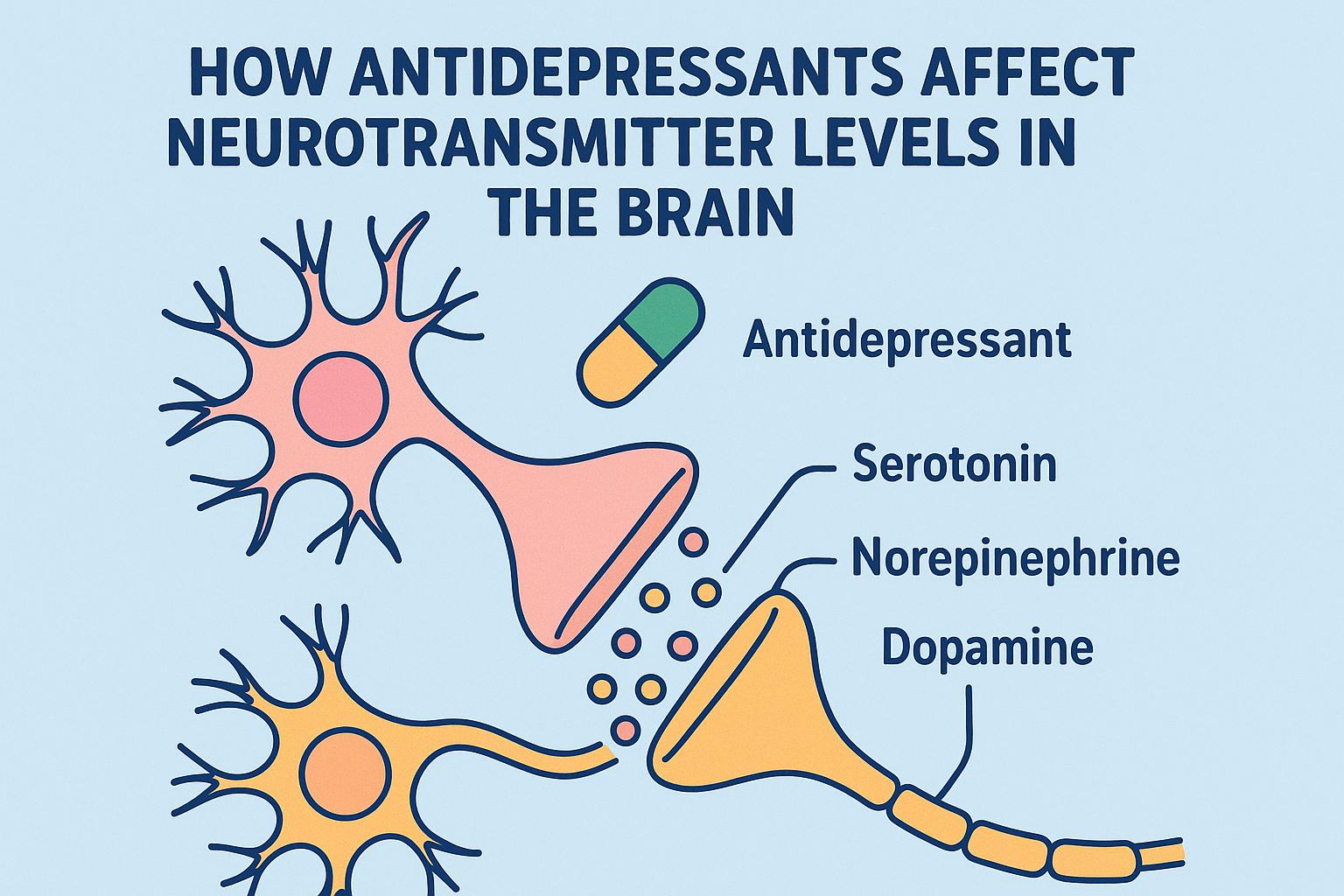
Opioids interact with the CNS by binding to specific receptors known as opioid receptors, which are distributed throughout the brain, spinal cord, and other areas. These receptors are part of the broader G-protein coupled receptor family. The interaction results in the modulation of pain signals and can induce feelings of euphoria. This makes opioids effective analgesics but also highly addictive.
At the heart of their interaction lies the opioid receptors. These receptors, primarily the mu, delta, and kappa receptors, are located in key regions of the CNS and other bodily systems. The mu opioid receptor, in particular, is most strongly associated with the analgesic effects of opioids as well as their addictive potential. When an opioid binds to these receptors, it causes them to undergo a conformational change.
Molecular Mechanisms
Upon binding, opioids inhibit the release of neurotransmitters by decreasing the intracellular concentration of cAMP, leading to reduced neuronal excitability. This process effectively dulls the sensation of pain, but also influences other neurological processes such as mood and reward. The inhibition mechanism involves complex sequences of intracellular events and results in dampened neuronal activity, thus diminishing the transmission of pain signals from nociceptors to the perception centers within the brain.
The reduction of cAMP levels not only affects pain perception but also intersects with pathways associated with mood regulation and the reward system, thereby contributing to the euphoric feelings often reported by opioid users. This dual effect—analgesic and euphoric—is what underscores both the medical utility and the abuse potential of these substances.
Short-term Effects
In the short term, opioids can offer potent pain relief and sedation. The efficacy of opioids in these roles stems from their direct action on the CNS to inhibit pain signal transmission. Analgesia, a state of decreased pain perception, is a primary reason for the clinical use of opioids, especially in post-operative care and severe injury scenarios. Despite their short-term benefits, these substances concurrently suppress the CNS leading to not only pain relief but also unintended adverse effects.
Among the most pressing of these side effects is respiratory depression, a condition arising from the diminished responsiveness of the brainstem’s respiratory centers to increases in carbon dioxide levels in the blood. With higher doses of opioids, the possibility of respiratory depression intensifies, necessitating vigilant monitoring when these drugs are administered medically.
Respiratory Depression
One of the most dangerous acute effects of opioid ingestion is respiratory depression. Opioids inhibit the brainstem’s response to carbon dioxide levels in the blood, compromising automatic breathing responses. The impact is dose-dependent and can be fatal without intervention. Timely medical response is imperative because untreated respiratory depression can quickly lead to hypoxia, where insufficient oxygen reaches the body’s tissues, potentially causing irreversible damage.
Long-term Effects on the CNS
Chronic opioid use engenders substantial shifts in the CNS, which may have enduring consequences. With sustained exposure to opioids, a user might develop tolerance and dependence, leading to an escalating cycle of use.
Neuroplasticity and Tolerance
Neuroplasticity is the brain’s ability to reorganize itself by forming new neural connections. With long-term opioid exposure, the brain adapts to maintain neurotransmitter balance, diminishing the drug’s analgesic potency over time. As the body becomes tolerant, larger doses are required to achieve the same pain-relieving effects experienced initially. This physiological adaptation is a double-edged sword: while it reflects the brain’s innate adaptability, it also underpins the perilous trajectory towards dependence and habituation.
Tolerance and neuroplasticity can also complicate efforts to manage chronic pain effectively. For patients reliant on opioids, increasing dosages heighten the risk of adverse effects without guaranteed pain relief.
Cognitive and Behavioral Implications
Beyond physiological changes, chronic opioid use intersects with cognitive functions, often leading to memory impairment, attention deficits, and diminished executive function. Such cognitive deficits impact an individual’s ability to perform daily tasks, undermining productivity and quality of life.
Compounding these cognitive challenges are behavioral shifts, such as anxiety, depression, and increased addiction risk. These conditions can exacerbate existing health problems, creating a cycle of opioid use and psychological distress that can be difficult to break. Moreover, addiction itself is a condition that exacts substantial social, economic, and personal costs.
Conclusion
Understanding the impact of opioids on the CNS is essential for balancing their therapeutic benefits against potential risks. Appropriately managing these potent medications requires a comprehensive understanding of their neurological interactions and the cascade of effects they can initiate. Scientific research, clinical studies, and ongoing education remain vital in optimizing opioid use, ensuring that these substances, while powerful, are wielded with utmost care and precision.
The complex interplay of biochemical processes, neuronal pathways, and psychological impacts underscores the need for informed application in medical settings and heightened awareness of the potential for misuse and dependence. As the medical community continues to unravel the intricacies of opioid interactions with the CNS, the emphasis must remain on patient safety, effective pain management, and minimizing the potential for abuse.