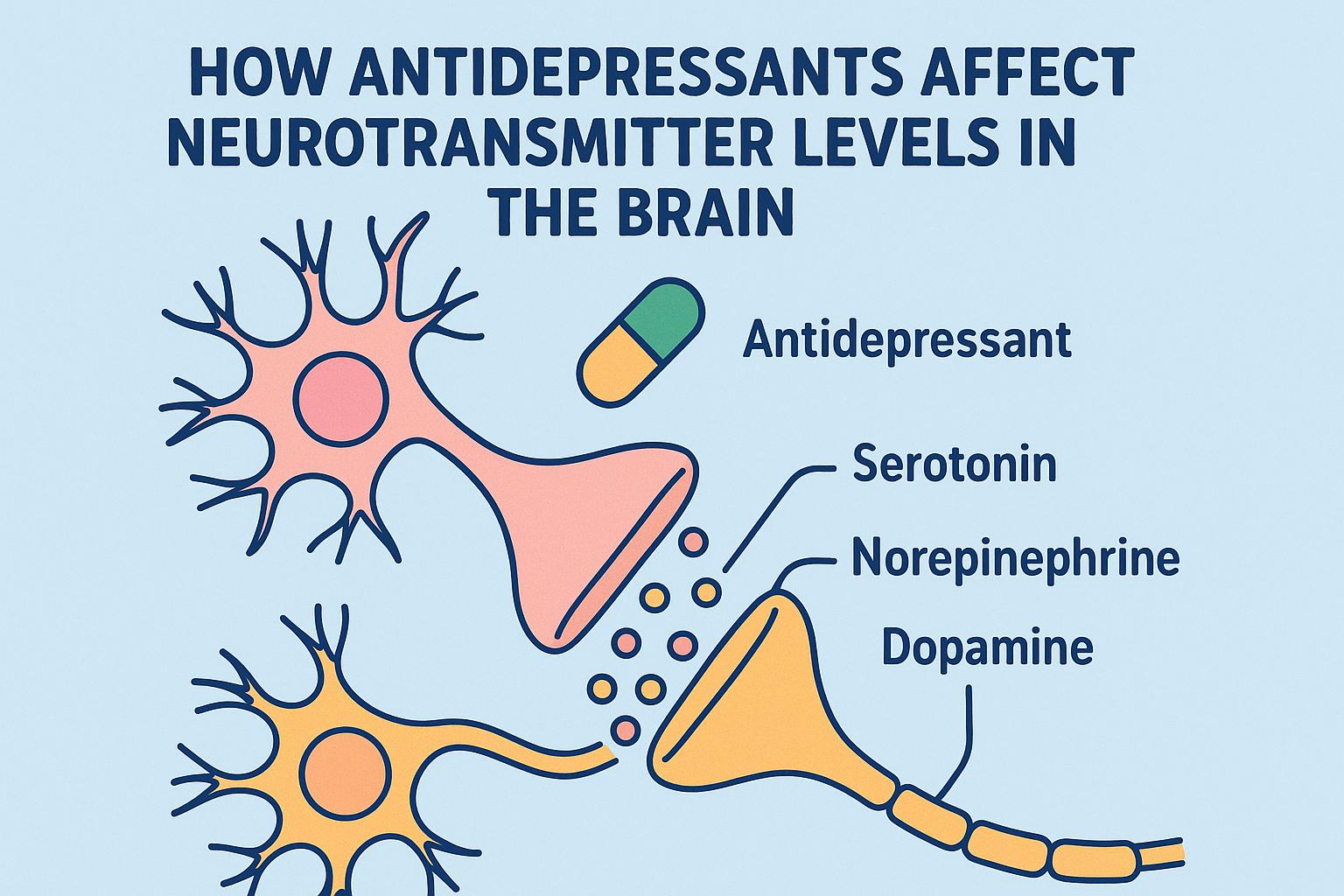
How antidepressants affect neurotransmitter levels in the brain.
Understanding Antidepressants and Neurotransmitter Levels in the Brain
Antidepressants play a crucial role in managing depression and related disorders. Their primary function is to alter the chemical balance in the brain, primarily affecting neurotransmitters, which are the brain’s chemical messengers. This article explores how different classes of antidepressants can influence neurotransmitter levels.
The Role of Neurotransmitters
Neurotransmitters are pivotal in transmitting signals between neurons, the brain’s nerve cells. They significantly impact mood regulation, emotional responses, and a range of mental functions. Three neurotransmitters are especially relevant when considering the effects of antidepressants: serotonin, norepinephrine, and dopamine.
Serotonin is involved in mood regulation and emotional well-being. Imbalances in serotonin levels are often linked to depression and anxiety disorders. The intricate role serotonin plays in modulating emotions is critical for mental health, and thus, its levels directly influence how we perceive our environment and experience emotions. Enhanced understanding of serotonin’s function has allowed development of medications targeting its pathways to mitigate effects associated with lower serotonin activity, often evident in depressive states.
Norepinephrine influences alertness and arousal. It plays a role in the body’s response to stress and can affect overall energy levels. This neurotransmitter is indispensable when it comes to the physiological underpinnings of the fight-or-flight response. Modern research underscores norepinephrine’s role in maintaining focus and cognitive performance, shining light on its broader impact beyond mood regulation.
Dopamine affects motivation, pleasure, and reward mechanisms in the brain. It is also integral to attention and learning processes. Critical to understanding human behavior, dopamine dysregulation is linked to myriad mental health conditions beyond depression, including addiction and certain personality disorders. Thus, targeting dopamine through medication aims not only to alleviate depressive symptoms but also improve cognitive and motivational deficits.
Selective Serotonin Reuptake Inhibitors (SSRIs)
SSRIs are the most commonly prescribed class of antidepressants. They work by blocking the reuptake of serotonin, leading to an increase in its concentration in the synaptic cleft. This heightened serotonin level can help improve mood and reduce symptoms of depression. Common SSRIs include fluoxetine and sertraline. They have set a benchmark in depression treatment due to their targeted action coupled with a favorable side effect profile.
By maintaining higher levels of serotonin in the brain, SSRIs can systematically counteract the pervasive feelings of sadness and anxiety that characterize depressive episodes. Additionally, they are recognized for their relative ease of administration, typically taken once daily, which simplifies adherence to medication schedules essential for effective mood stabilization.
Serotonin-Norepinephrine Reuptake Inhibitors (SNRIs)
SNRIs function similarly to SSRIs but target both serotonin and norepinephrine. By preventing the reuptake of these neurotransmitters, SNRIs can address a broader range of depressive symptoms. Examples of SNRIs are venlafaxine and duloxetine. These medications offer therapeutic advantages by simultaneously addressing mood dysregulation and issues related to alertness and arousal.
The dual action of SNRIs positions them as versatile options for individuals who may not respond optimally to SSRIs. Their broader mechanism allows them to also be beneficial for conditions such as certain anxiety disorders and neuropathic pain, expanding their utility beyond depression treatment.
Norepinephrine-Dopamine Reuptake Inhibitors (NDRIs)
NDRIs, such as bupropion, specifically inhibit the reuptake of norepinephrine and dopamine. This class of antidepressants is often used when SSRIs do not provide sufficient relief or when preserving sexual function is a concern, as they have a different profile of side effects. We see the role of NDRIs widening not only within the purview of depressive disorders but also in addressing symptoms of attention-deficit/hyperactivity disorder (ADHD) and smoking cessation support.
Their ability to modulate neurotransmitter levels without significant sedative effects makes them an appealing choice for patients encountering fatigue and low energy as primary symptoms associated with depression.
Tricyclic Antidepressants and Monoamine Oxidase Inhibitors
Tricyclic antidepressants (TCAs) and monoamine oxidase inhibitors (MAOIs) are older classes of antidepressants. They are less commonly used today due to their side effect profiles. Despite this, they remain crucial for understanding the evolution of depression treatment.
TCAs block the reuptake of serotonin and norepinephrine, offering a potent means of alleviating depression symptoms. However, their broader action across multiple neurotransmitter systems can lead to undesired side effects, necessitating careful therapeutic monitoring.
MAOIs inhibit the breakdown of neurotransmitters by blocking the activity of monoamine oxidase, an enzyme. They offer alternative treatment efficacy particularly in cases of atypical depression or for patients unresponsive to other medications. A significant aspect of their usage includes dietary restrictions, to prevent hypertensive crises which have historically limited their easy adoption in mainstream pharmacotherapy.
Conclusion
Antidepressants have a profound impact on the neurotransmitter levels in the brain, which contributes to their efficacy in treating depressive disorders. By altering the balance and availability of neurotransmitters, these medications can help restore emotional stability and improve quality of life. Understanding their specific mechanisms enables patients and healthcare providers to tailor treatments more precisely to individual needs.
When considering antidepressant treatment, it is crucial to understand these mechanisms and consult healthcare professionals for personalized medical advice. This dialogue ensures an accurate assessment of benefits versus risks and considers personal health factors, prioritizing both efficacy and safety in managing depression.
For more information on the topic, you may explore detailed articles available on Mayo Clinic or National Institutes of Health. These resources can provide further insights into mental health treatments and advancements in antidepressant therapies. Enabling continuous learning and understanding of these medications promises not only to enhance treatment outcomes but further destigmatize mental health conditions and their management.